Fuente: Vulvodyinia - Who, What, Why?
« Descargar documento (formato PDF) »
"But I've never seen it !!!"
Outline for discussion
Is vulvodynia rare?
No longer considered a "rare disease"!
Web survey re: vulvar pain
Vulvar Pain: Web survey
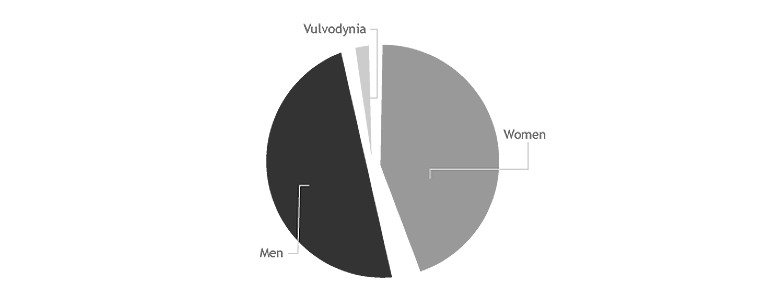
What is vulvodynia?
"Vulvodynia" coined in 1983 by International Society for the Study of Vulvovaginal Disease (ISSVD)
What is it?
15 women in each Family Physician's practice at least double that in Each Gynecology practice 2,400,000 women in the United States
Making the diagnosis
Exclusions
Other causes of vulvar pain or symptomatology
Other causes of vulvar pain or symptomatology
Definition evolution
Categorization of vulvodynia
Occasional erythema in that area.
Who gets vulvodynia?
Women have had YEARS of pain prior to diagnosis:
Number of previous physician seen for vulvar pain
Who are patients seeing?
Just how bad can it be?
Activities that worsen then pain
Activities that reduce the pain
Data about sexuality of women with vulvodynia are compelling
Marital Status
Sexual activities in the past month
But…. There are negative findings as well:
Women with vulvodynia rate themselves MORE NEGATIVELY as sexual people than did controls.
But what Causes it?
Our data:
Marital satisfaction
Beck Depression Inventory
Perception of Sexual Activity
Sexual abuse
Our data: Sex abuse – personal or family
Toxins?
Immunologic?
Pelvic floor muscle impairment
Related to interstitial cystitis?
Sensory Processing Alteration? Similar changes in periphery! Summary of causality
Treatment – what can we do?
Treatment options: Often used, but appear ineffective
Treatment options – appear to be beneficial
Amitryptiline (Elavil)
SSRIs
Gabapentin (Neurontin)
Biofeddback and physical therapy
Cromolyn sodium cream
Calcium citrate
Surgery – vestibulectomy
Recent data (2001 – Bergeron)
Surgery – Laser of vulva
Summary of treatment
Take home lesson












